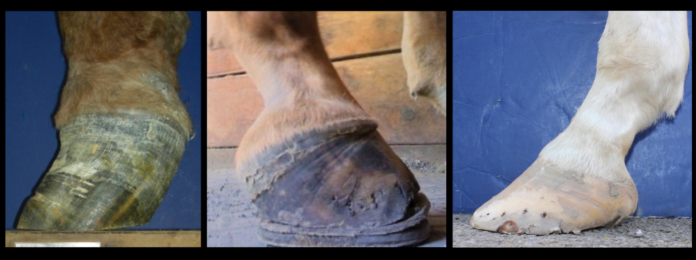
There is so much about the foot we are expected to interpret from external landmarks: sole depth, toe length, heel height, position of the bones, soft tissue inside the capsule, and more! Most of us hoof care providers can get really close in our assessment of the feet we work on, however, we all have some percentage of our horses that we feel a little less certain about. It might be a horse with very distorted feet, or a specific pathology that muddies the waters a bit.
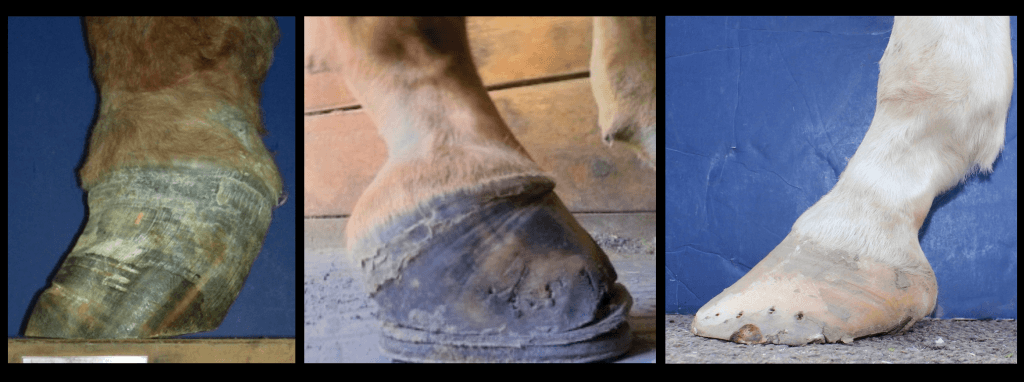
In these cases, hoof radiographs (x-rays) can be quite enlightening. The information a well taken hoof radiograph can give you is tremendous, especially with pathology or severely distorted feet. Although I’m also surprised at how helpful radiographs of my healthier feet can be – just a slight adjustment made from seeing a radiograph can make a big difference to the horse.
So what do you need to get good information out of radiographs to help you in your hoof care work? There are two main views that are most helpful to the hoof care provider:
- Lateral-Medial, from the side of the foot, also known as a Lateral Radiograph
- Dorso-Palmar, from the front of the foot, also known as a DP or AP Radiograph
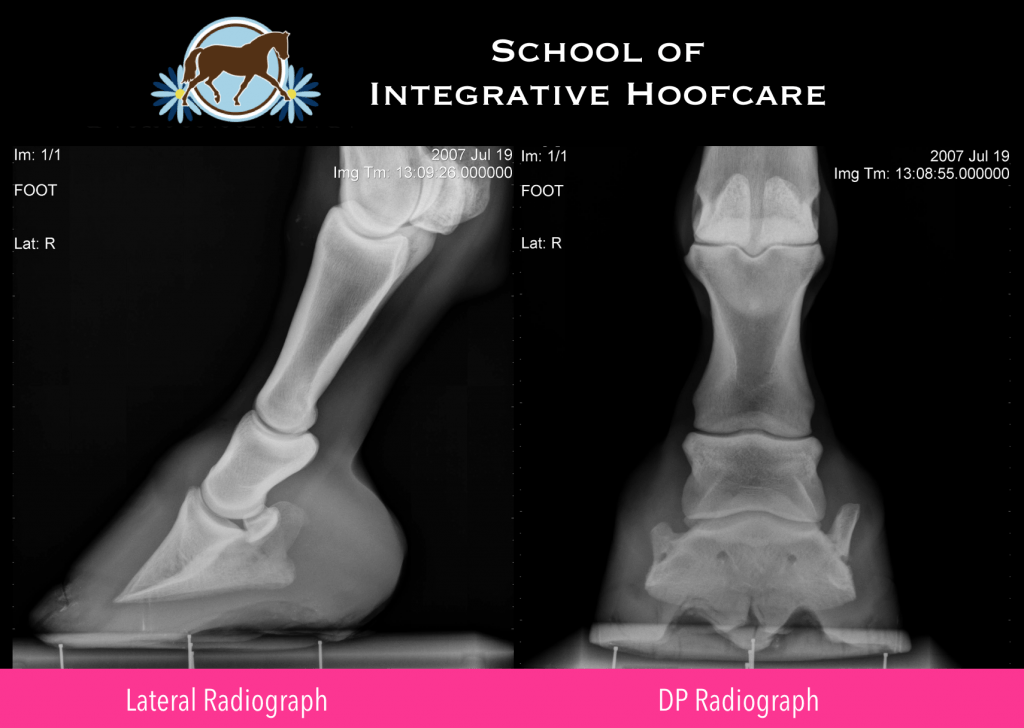
Here are several key elements that will help you be successful assessing Lateral and DP radiographs for your hoof care work:
1. Be present when the radiographs are taken. You’re going to want to ensure the radiographs are taken with technique that makes them accurate and usable for hoof assessment. If you cannot be present, you’ll want to have a conversation with the veterinarian as to what you’re looking for and how you want the foot marked or labeled.
2. The horse’s feet need to be picked out and wire brushed clean, including the hoof wall from ground surface to the coronary band, around the heels, into the collateral groves, central sulcus, and any other separations and pockets, for clear visibility of all structures in the radiograph. Many of the tips and tricks in my previous blog on taking hoof photographs also apply to taking good radiographs.
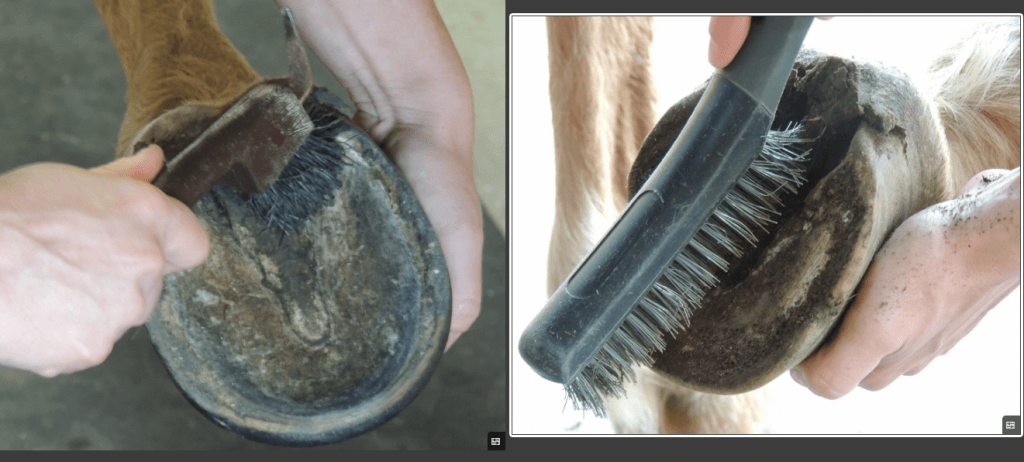
3. The horse needs to be standing on level ground, with cannon bones perpendicular to the ground, a leg at each corner. Both feet, whether front or hind, need to be on blocks of equal height, and the horse’s head should be facing straight ahead. This prevents body positioning and weight bearing imbalances from skewing your radiographs.

While good setup and technique for acquiring the radiographs is critical for any assessment of the horse’s foot, it is equally important they are taken with a scale marker for calibration so physical measurements can be achieved that are accurate.
There are several options for calibrating radiographs, three of which are shown here: EPC Solutions Scale Marker, a wire on the dorsal wall of known length, and the Metron Imaging Blocks. Scale markers need to be in the “plane of interest” which would be the area of the subject that is most important to scale to. In this case, that would be the mid-line of the limb.
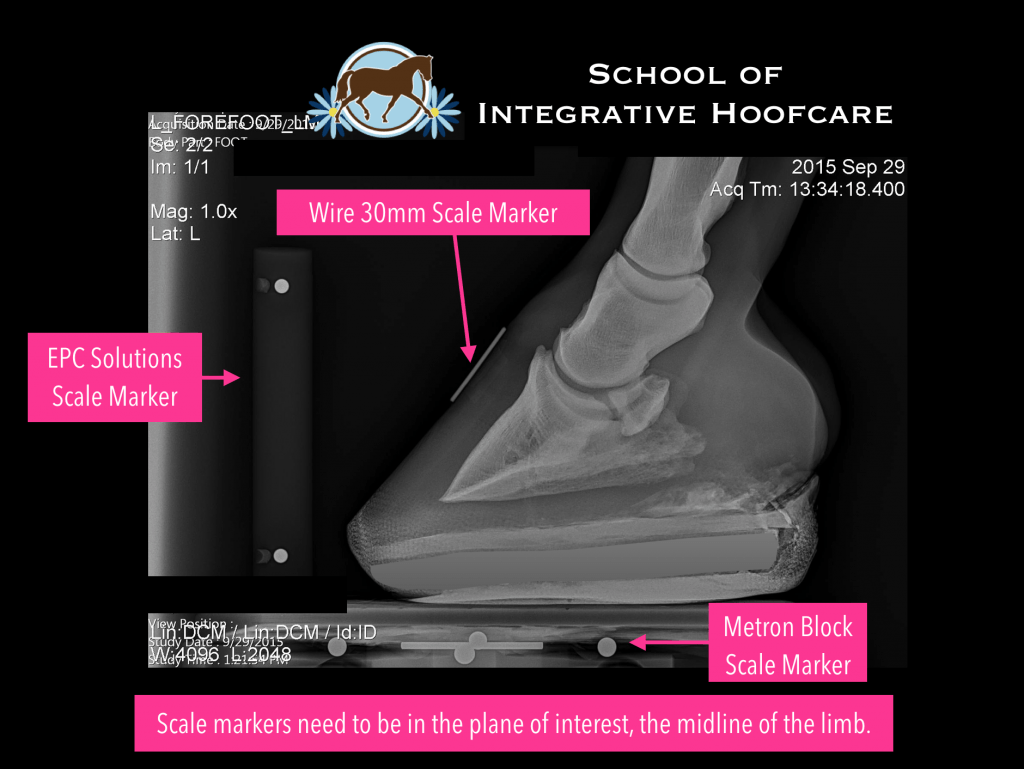
There are also other markers that can be helpful like a thumb tack at the true frog apex, or at the widest part of the foot on the frog. Barium radio-opaque paste showing the true dorsal wall and heel on lateral radiographs is often helpful as well.

Here are some examples of radiographs with common problems that make it challenging to assess hoof parameters.
In this image, there are no scale markers, and the foot is not entirely included in the radiograph:
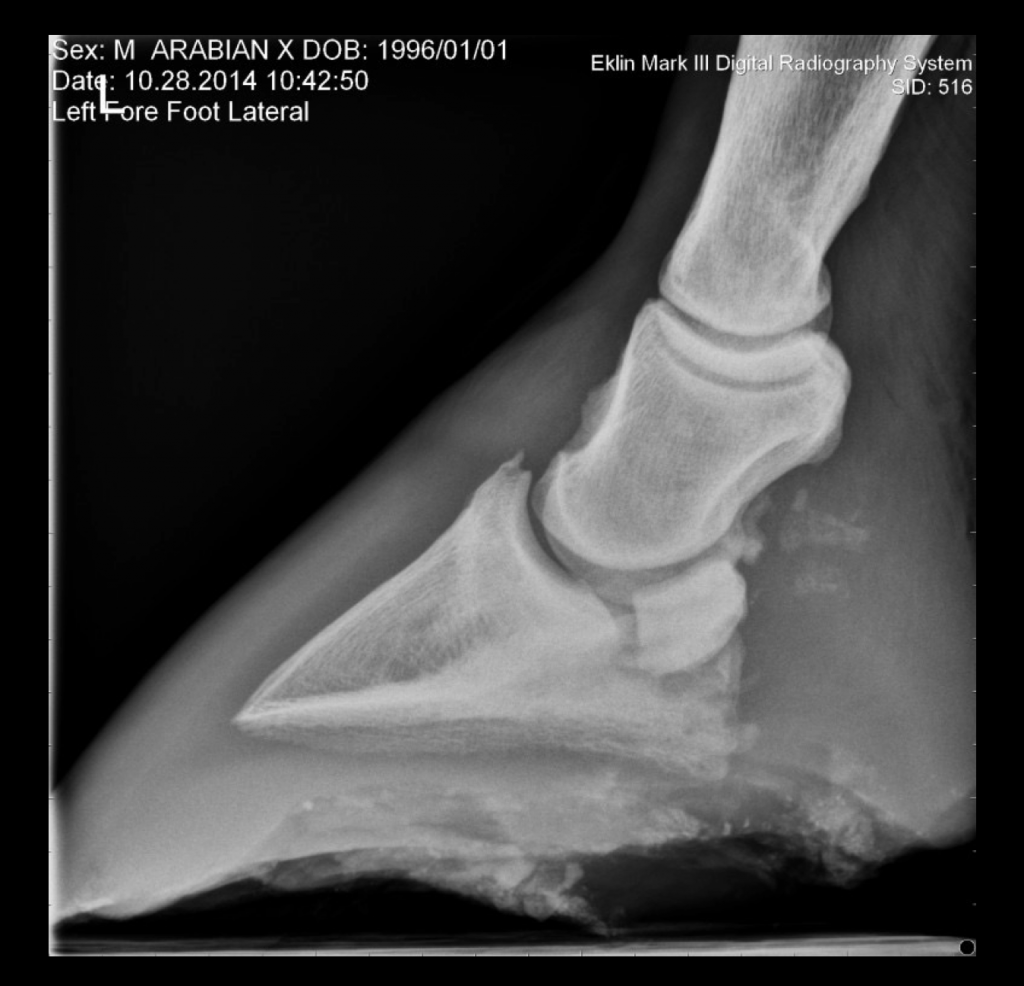
This radiograph is not a true lateral view, it was taken off-axis and without scale markers:
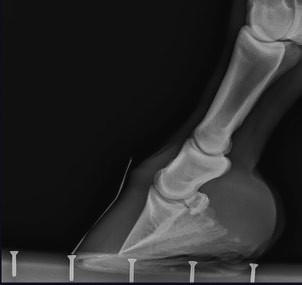
Well taken hoof radiographs can be so helpful to the hoof care provider in providing accurate information for helping the horse. To appreciate how powerful this information can be, EPC Solutions, a leading innovator in Equine Podiatry Consulting, utilizes Equine Podiatry X-rays as an integral tool in their practice. They assess the distal limb and develop farrier plans that optimize recovery in cases with difficult hoof pathology. Here is what they have to say about taking hoof radiographs for the farrier:
“There are significant differences between diagnostic radiograph views compared to podiatry views. Diagnostic radiographs are usually aimed at an angle to the sagittal plane, investigating into a joint or at oblique views to “see around the corner”. They are shot with a harder exposure that burns out edge definition and soft tissue detail. Diagnostic views incur magnification and image distortion but are not usually an issue for intended purpose.
For podiatry radiographs the x-ray beam should be aimed straight-on, perpendicular, to the distal limb and the crosshairs centered strategically at or near the bottom edge of the coffin bone. It is important to shoot the image with a level beam- running on a horizontal plane to the ground surface/palmar rim of the hoof. Generally, due to the height of the x-ray unit body, this is not possible unless we raise the hooves – typically placing them on wooden blocks to align the bottom of the coffin bone level to the height of the beam.
Combined with a thorough understanding of hoof bio-mechanics, distal limb pathology, farriery, nutrition and body therapy support, podiatry x-rays provide very useful information for veterinarians and hoof care providers towards a complete distal limb solution.”
Here is an example of what good podiatry radiographs can do for you, as marked up by EPC Solutions.
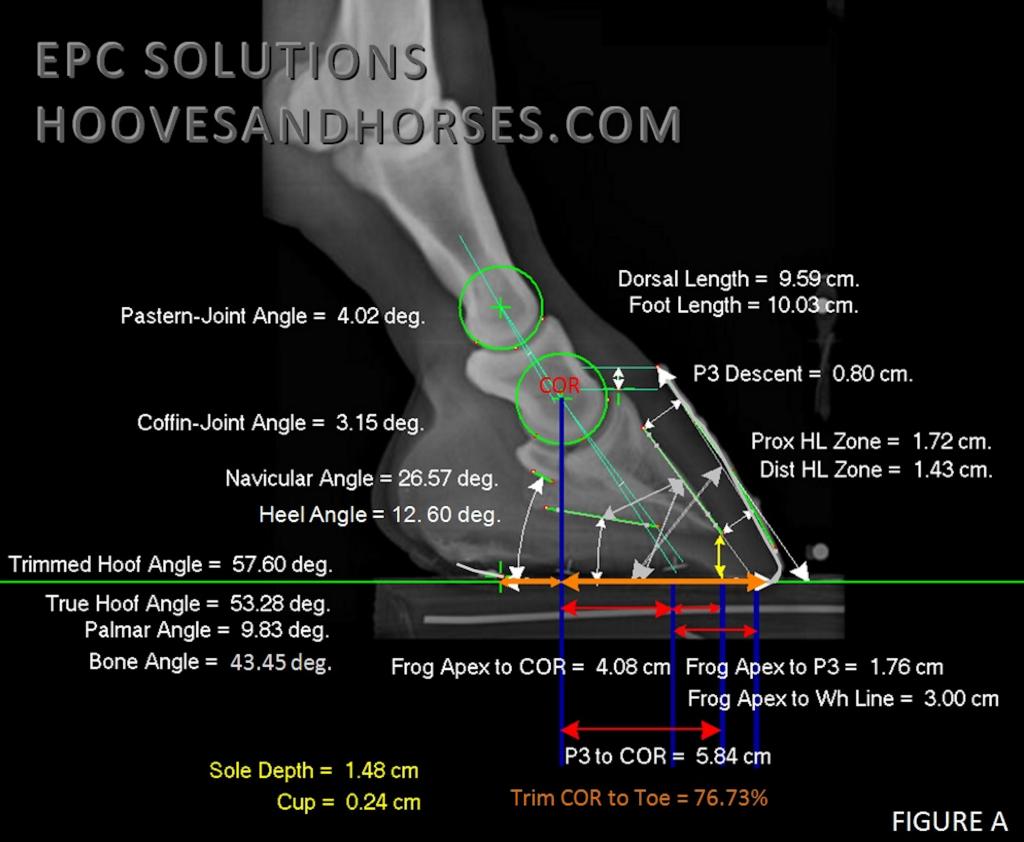
“Podiatry x-ray hard and soft tissue parameters provide useful insights into distal limb health and static balance. While externally this hoof may appear relatively healthy and even nicely aligned with hoof pastern axis, many internal data markers highlight the need to optimize the hoof balance and address possible underlying metabolic changes in the hoof before long-term pathology affects soundness levels”. EPC Solutions
Ideally, we would all get baseline podiatry radiographs of our horse’s feet for assessment once a year to have a greater chance of preventing lameness issues before they occur. However, even if you just get well-taken, measurable radiographs of your difficult cases, the horses will benefit immensely.
Stay tuned for Part 2 next month, which will discuss how to read your accurately acquired, measurable radiographs.