This is a snippet from my upcoming DVD, Fighting Founder. I’ve also recently released a trimming video featuring some of the lucky rescue horses at Laughing Pony Rescue in Rancho Santa Fe, California.

DVDs are available for sale on my website here:
Onset – Acute Stage
Immediate Action
The onset of most laminitis cases is rapid. It’s critical to act quickly if you want to minimize lamellar damage. By the time the owner calls you to come look at the horse, it may be too late to implement damage control in the form of an ice boot. But in the event that you see the horse within hours of symptoms, or for horses who have, for example, indulged in a grain overload and have not yet presented with symptoms, icing the leg from the knee down, preferably with crushed ice, can minimize lamellar damage. The icing should continue for 24 hours after the horse’s digital pulses and rectal temperature return to normal.
PinPointing the Trigger
The next most critical step is to determine the underlying cause. This is relevant for both acute and chronic cases. There are many potential triggers – among them: inappropriate diet/insulin resistance or EMS; obesity; Cushing’s disease; contralateral limb laminitis (think of Barbaro). Steroid therapy is also a common trigger.
The most common cause I see in the field is simply inappropriate diet, with high carbohydrates, and frequently, obesity. Because of this, I generally recommend putting the horse on an “emergency” diet of low carb grass hay and nothing else until the cause is resolved.
Bloodwork must be done to arrive at an actual diagnosis of Equine Metabolic Syndrome or Insulin Resistance. Make sure the testing includes both a hormone assay to establish insulin levels, and glucose levels; it is the ratio between the two that will give you the most accurate information. Dr. Eleanor Kellon’s Equine Cushings and Insulin Resistant website and forum will walk you through this part, and provide invaluable assistance in formulating an appropriate diet.
If you believe the trigger was not somehow diet related, there may be a need for antitoxin therapy, or other vet prescribed medication necessitated.
Form Your Trimming Plan
You’ll want good, properly marked digital radiographs right away to help you form a trim plan.
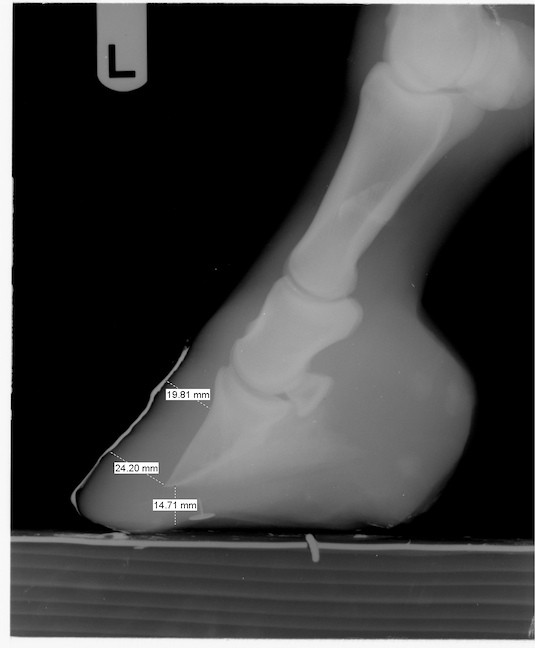
An appropriately marked radiograph
Establishing an appropriate palmar angle is important, but can be tricky. If the horse has a poorly developed caudal foot, chronic thrush, or extremely high heels, you’ll need to approach this with caution. The protocol put together by Pete Ramey and Dr. Debra Taylor at Auburn University prescribes no more than 10mm change to palmar angle at one trim, but even this much can be too much at once for some horses.
There’s also the question of whether taking too much heel causes the deep digital flexor tendon to pull on P3. Many vets still insist this is true, and I’ve battled heel height on some founders to the point where I’m still on the fence about this subject. At any rate, it is something to take into consideration.
Finding the point of breakover is critical. How to best implement that breakover is a source of some debate. I’m going to tell you what has worked the best for me.
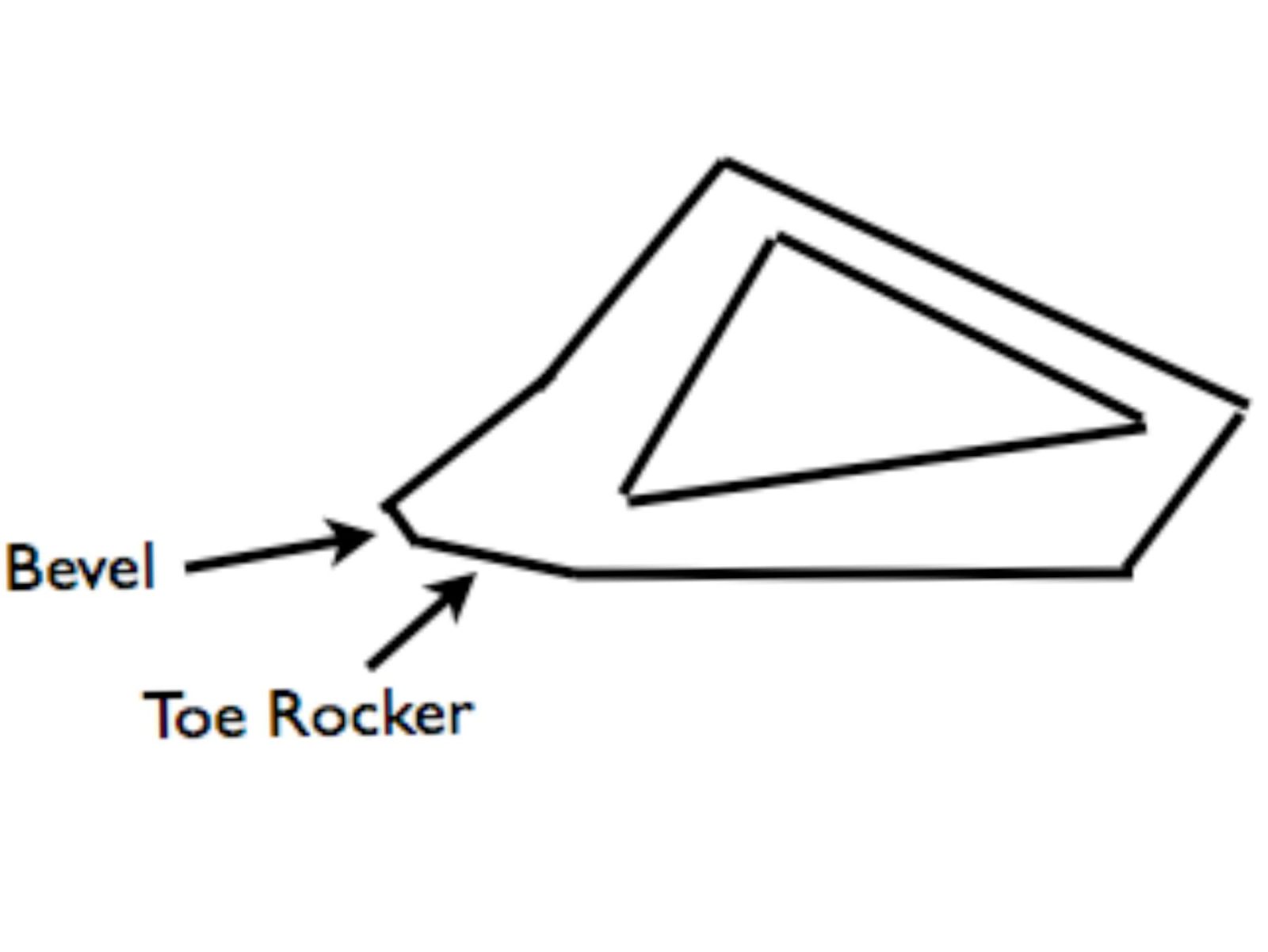
Using the digital radiographs, I follow the dorsal aspect of P3 to the bottom of the foot in a line. From that point forward, I apply about about a 10 degree rocker to the toe from toe pillar, or toe corner, to corner. I finish the toe by beveling back just as you would a healthy foot – within an eighth of an inch of the apparent white line, and not into lamellar wedge.
Choose hoof protection that keeps the horse as comfortable as possible. Early on, this might be the Easyboot Rx. Further into the transition, as the horse begins to move around more confidently, Easyboot Epics, Edge boots, and Gloves all work well. Hoof casting with Equicast casting tape is another excellent approach, and may be easier and more effective for absentee owners, boarding facilities, and horses ambulatory enough to be turned out on a dry lot pasture.




